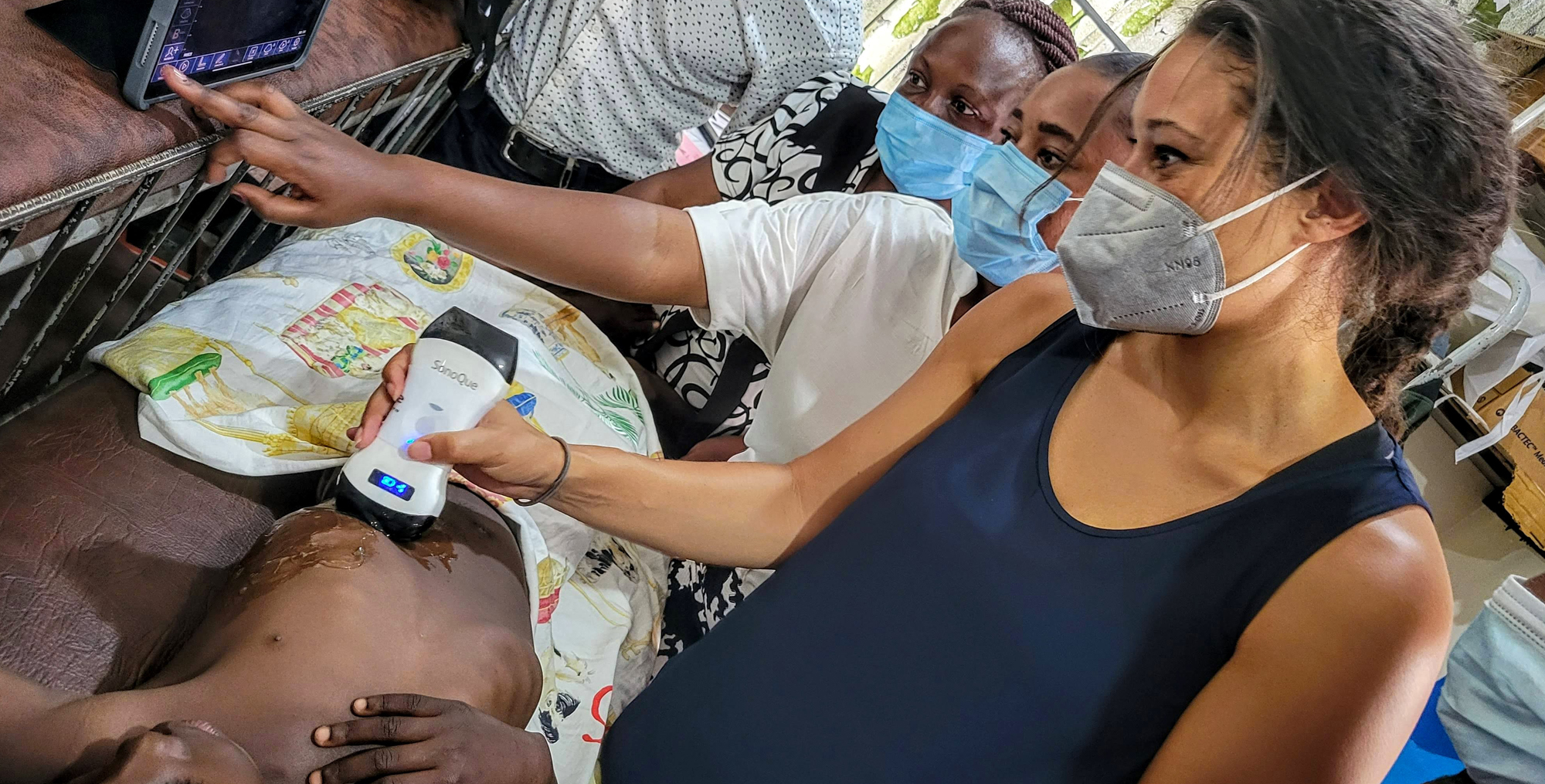
Above: Dr. Alexandra Power-Hays delivers care to a pediatric patient in Uganda. Photo courtesy of Dr. Alexandra Power-Hays.
Physician scientists bring critical insights from interactions with patients to their clinical research, making unique and important contributions to the advancement of human health. It is with recognition of this vital role in the field that the Doris Duke Foundation has long supported their career-advancing clinical research through programs such as the Clinical Scientist Development Award and Physician Scientist Fellowship.
If ever you wanted an instructive example of what that value looks like in practice, one might simply turn to Dr. Alexandra Power-Hays, a 2021 Doris Duke Physician Scientist Fellow now in her fellowship training in pediatric hematology and oncology at Cincinnati Children’s Hospital Medical Center. For Dr. Power-Hays, these direct experiences with patients not only inform her scientific observations and questions but fuel her interest in and commitment to a career in medical research.
“Starting out, I thought I wanted to be a doctor and that was it, but then you see patients, you start to see patterns and start to ask questions,” said Dr. Power-Hays. “I wanted to answer those questions in a bigger way and see how things can apply to more children and have a wider impact. So, being a doctor is the root of my scientific endeavors. My aspiration is to have both a clinical and a research practice, and to hopefully do some patient advocacy through my research.”
As a physician scientist studying and treating children with blood disorders, Dr. Power-Hays became particularly interested in sickle cell disease and the disparities she saw in how it was treated. Unlike patients of diseases such as hemophilia and cancer, teens with sickle cell disease who communicate their pain are too often not believed, she said, and systemic and financial inequities can provide barriers to accessing therapies for the disease. Those barriers can have profound consequences. Sickle cell disease causes healthy round blood cells to take on a sickle shape, clogging veins and arteries, and blocking blood flow to organs. When not treated with the right level of control, she explained, sickle cell disease patients describe “excruciating pain that feels like hammering or drilling into your bones, things that just sound horrible.”
With this noted, Dr. Power-Hays has seen firsthand how transformational the right treatments can be for patients suffering from the disease. One of the most successful and cost-effective approaches to treating sickle cell disease was pioneered by Dr. Power Hays’s mentor, Dr. Russell Ware, to provide hydroxyurea, a medication that helps red blood cells stay rounder, to patients at the maximum tolerated dose without overdosing. Getting to this optimum level, she said, requires bringing children back every few months and slowly increasing the dose.
Dr. Power-Hays noted that patients on perfect, customized doses of hydroxyurea have so few complications or symptoms of pain that they can almost forget they have a chronic disease. In many places, however, and particularly in Sub-Saharan Africa, “where it might take a family’s entire month’s salary to get their child to a clinic," it can be a logistical challenge to get patients to clinics to adjust the dosage and so they get parked on a fixed, standard dosage, which can mean fewer clinical benefits or higher levels of toxicities for children. The consequences can be substantial. In addition to causing debilitating pain, sickle cell disease can result in early death. In Sub-Saharan Africa, sickle cell anemia contributes to an estimated 5-16% of the under-five mortality rate.
Awareness of this issue sparked a research question for Dr. Power-Hays: What if they could determine the right hydroxyurea dosing algorithm for children with sickle cell anemia in Uganda? In the United States, this approach has been shown to be safe and accurate for determining a patient’s optimal hydroxyurea dose with less frequent monitoring and fewer drug-related toxicities, but the safety and feasibility of this technique has never been assessed in a low-resource setting, such as the one in which she proposed to situate her study.
This is the premise of the research Dr. Power-Hays is pursuing under Dr. Ware’s mentorship with her Physician Scientist Fellowship grant from the Doris Duke Foundation. If successful, Dr. Power-Hays’s study could result in removing barriers to the use of the most effective, disease-modifying therapy widely available to children in Sub-Saharan Africa. If the strategy can be implemented in Uganda, it would decrease logistical burdens that too often prohibit effective dose escalation and monitoring. In addition, studies have shown that increasing hydroxyurea treatment of sickle cell disease decreases the number of blood transfusions required for the patient population. Given that blood transfusions are a shared and scarce resource, Dr. Power-Hays noted that this could allow for additional saved lives, a ripple effect that could be persuasive to public health officials and policymakers.
The powerful potential impacts of this work, along with the strength of her rigorous research proposal, her documented academic and early-career accomplishments, mentorship and the compelling vision she shared for her future as a physician scientist, were among the multitude of reasons that a panel of accomplished physician scientists selected Dr. Power-Hays for one of nine 2021 Doris Duke Physician Scientist Fellowships. Yet, Dr. Power-Hays revealed that she initially felt a bit intimidated at the prospect of vying for such a competitive award, before reflecting on a piece of advice she was given during her residency by another hematologist, Dr. Natasha Archer. Dr. Archer told her, “Be the applicant. Don’t be the judge.”
“It’s not your job to pre-decide if you’re going to get it or not,” Dr. Power-Hays counseled others who may be feeling a similar sense of intimidation. “It’s just your job to look at the application and try your best, and if you put it all together and connect with somebody who can help and give you some advice and then go for it, you’re not really losing anything. Instead, you’re gaining the connection you made with a mentor; you’re gaining the career development plan that you laid out; you’re gaining a project that’s crafted and you can maybe seek other sources of funding. You only have things to gain by applying whether or not you receive the grant.”
Dr. Power-Hays expressed relief that she pushed past her momentary hesitancy and went for the opportunity. She noted that the mentorship, the funding, the network and the chance to pursue research that could have a significant effect on children with a debilitating disease are all aspects of the Physician Scientist Fellowship that she considers deeply valuable as she builds her research career.
“I’m very fortunate that I was able to get this award to work with this mentor, who has had a career of improving care through research in an amazing way,” said Dr. Power-Hays. “I hope to build on that legacy. I want to ask and answer questions through my research in a way that creates buy-in and motivates clinicians, government officials and policymakers to support and apply evidence-based practices. This project is a good example of where I have an opportunity to examine how we can reduce logistical challenges to get the biggest benefits out of an essential treatment. Through providing the evidence base, we can help a minister of health, for example, better implement solutions that could transform the lives of a vast number of children and families.”